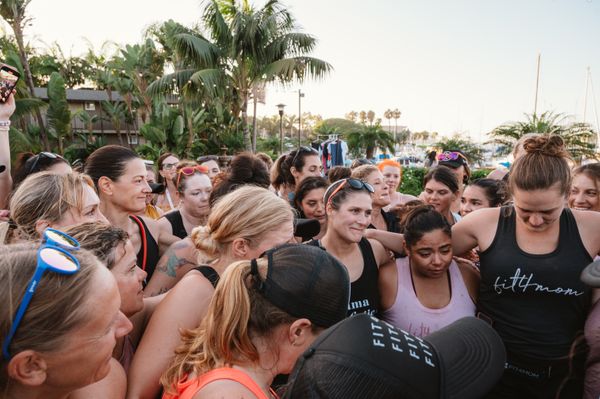Social support is equally critical. “Friends and family can help by doing simple tasks like holding the baby so parents can nap, shower, or take a walk,” Adrienne suggests. And support groups—whether online, in-person, or through organizations like FIT4MOM—can be lifelines. “FIT4MOM played a key role in my recovery. I met wonderful friends, had something on the calendar to get me out of the house, and exercised outdoors, which gave me a sense of purpose.”
For some parents, professional help is needed, such as counseling to navigate the challenges of new parenthood or even medication to treat mental health conditions. Adrienne reminds us that “any decision about medication should always be made in consultation with health care providers.”
Adrienne offers practical advice for those who want to support new parents:
- Ask how they’re doing. Focus on the parent’s well-being, not just the baby’s.
- Normalize their experience. Let parents know they are not alone and that many struggle during this transition.
- Offer help. Cook a meal, fold laundry, or care for the baby so parents can rest.
- Connect them with support:
In times of crisis and moments when mental health needs urgent attention, it is crucial to have readily accessible resources. Whether you or someone you know is facing an emergency or navigating the complexities of mental health, a network of support is available. The following resources serve as lifelines, offering immediate assistance and guidance.
From local emergency rooms to national hotlines, these contacts are here to provide the necessary support. Remember, seeking help is a sign of strength, and these resources are designed to offer hope, understanding, and assistance when it's needed most. In times of distress, don't hesitate to reach out and connect with the compassionate professionals dedicated to supporting individuals and families on their mental health journey.
In an Emergency
Go to your local emergency room.
Suicide and Crisis Lifeline: Dial 988
National Crisis Text Line: Text HOME to 741741 from anywhere in the USA, anytime, about any type of crisis.
National Suicide Prevention Hotline and Website: 1-800-273-8255 & suicidepreventionlifeline.org
National Alliance on Mental Illness (NAMI) Helpline: NAMI offers a Helpline that provides information, resources, and support for individuals and families dealing with mental health conditions. Call 1-800-950-NAMI (6264) for assistance.
National Maternal Mental Health Hotline: Counselors provide information, support, brief interventions, and resources: 1-833-TLC-MAMA (1-833-852-6262) - Call or text, 24/7, English and Spanish
National Domestic Violence Hotline: The National Domestic Violence Hotline offers confidential support for individuals experiencing domestic violence. Call 1-800-799-SAFE (7233) or chat online at www.thehotline.org for assistance.
Postpartum Support International (PSI): Postpartum Support International (PSI) is the world’s leading organization in providing hope and help to childbearing individuals affected by maternal mental health conditions, as well as their partners and families. Call 800-944-4773 or text 503-894-9453 www.postpartum.net